For decades, Polycystic Ovary Syndrome (PCOS) has been defined by its name—a term that implies a specific physical characteristic of the ovaries. However, modern medical research is revealing that the condition is not merely a gynecological issue, but a complex metabolic and genetic disorder that may also impact men.
The Misnomer: It Was Never About Cysts
The term “polycystic” is actually a historical misunderstanding. In the 1930s, physicians identified a cluster of symptoms—including infertility and irregular periods—and observed fluid-filled sacs on the ovaries during surgery. They labeled these “cysts.”
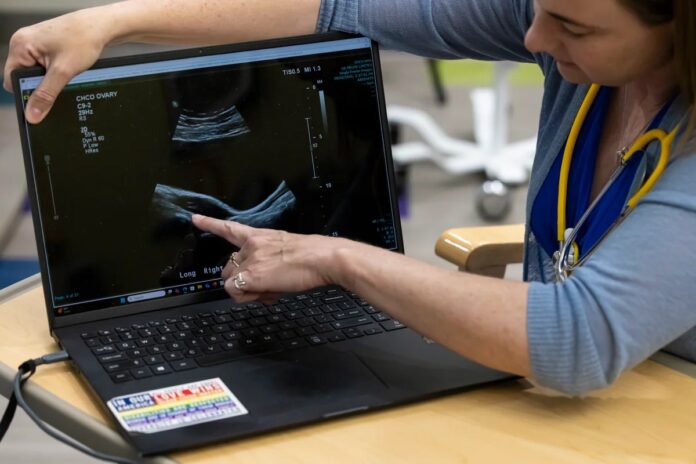
We now know these are not cysts at all, but follicles : underdeveloped eggs that failed to mature. Unlike true cysts, these follicles do not grow or rupture; they simply sit in the ovary, often appearing like a “string of pearls” on an ultrasound. By focusing on the location (the ovaries) rather than the cause, the medical community has long overlooked the true drivers of the syndrome.
The Root Cause: A Metabolic Connection
Current research suggests that PCOS is driven by a genetic susceptibility to insulin resistance.
The biological chain reaction works as follows:
1. Genetic Predisposition: A person is born with a higher risk of insulin resistance.
2. Insulin Resistance: The body’s cells do not respond effectively to insulin, causing the pancreas to overproduce the hormone to compensate.
3. Hormonal Disruption: High levels of insulin trigger the body to produce excess androgens (such as testosterone).
4. Symptom Manifestation: In women, these high androgen levels disrupt ovulation and cause symptoms like acne or excess hair growth.
Why This Matters for Men
Because this condition is rooted in genetics and metabolic dysfunction rather than just reproductive organs, it does not stop at the female anatomy.
Studies involving the male relatives of women with PCOS—such as brothers and fathers—have revealed striking patterns. These men often show:
– An increased risk of being overweight.
– A higher prevalence of metabolic syndrome.
– Elevated levels of certain male hormones produced by the adrenal glands.
Despite these findings, a significant gap in medical awareness remains. Most general practitioners are not trained to recognize these “PCOS-like” metabolic features in men, leaving a large population of patients undiagnosed and untreated.
The Push for a Name Change
Medical experts are now advocating for a complete rebranding of the condition. The goal is to move away from a name that describes a symptom (cysts) and toward one that describes the underlying mechanism (metabolic and hormonal dysfunction).
The benefits of such a change are backed by historical precedent. For example, when “Syndrome X” was renamed Metabolic Syndrome, research into the condition exploded because the name finally provided a clear, unified direction for scientists.
“If more funding was available… we would be able to have much better treatments and targeted treatments,” says Ricardo Azziz, a professor of reproductive endocrinology.
Currently, there is not a single FDA-approved drug specifically for PCOS. A name change could act as a catalyst, attracting the funding and research necessary to develop targeted therapies for both women and men.
Conclusion
By reframing PCOS as a metabolic disorder rather than a strictly gynecological one, the medical community hopes to improve diagnosis accuracy and unlock new treatments for the millions of men and women affected by this genetic condition.